
Diabetes Self-Management Education & Support (DSMES)
Discover how DSMES can deliver lifelong support as you strive to live healthy with diabetes.
DSMES Overview
What is Diabetes Self-Management Education and Support (DSMES)?
DSMES, also referred to as diabetes education, gives you the knowledge, skills and support to manage your diabetes. It provides you with the foundation to help you navigate your daily self-care with confidence and is provided by a diabetes care and education specialist, an experienced healthcare professional such as a registered nurse, registered dietitian, pharmacist and others who have gone on to specialize in diabetes.
Diabetes care and support is offered through DSMES programs (also called diabetes education programs) which can be found in hospital outpatient centers, clinics, physicians’ offices, pharmacies and wellness centers, to name a few. Many of these programs are accredited by ADCES®, which means the program has met vigorous criteria set by the U.S. Department of Health & Human Services.
What happens during DSMES?
During initial DSMES visits, your diabetes care and education specialist will spend time with you on developing a plan that helps you overcome potential barriers to managing your diabetes.
A diabetes care and education specialist can help you:
- Understand exactly what diabetes is and how it affects your body
- Discover how diabetes medications work
- Identify what types of food are best for you and how to plan meals that fit your lifestyle, culture, religious beliefs and budget
- Determine the best type of glucose monitoring device for your specific circumstances
- Find apps and other tools that offer reminders and help you track your progress
- Help you cope with stress and solve problems as they arise
- Interpret data from your diabetes devices to get treatment recommendations
Coverage & Participation
Medicare and most insurance plans cover DSMES, but it does require a referral from your doctor, nurse practitioner or PA (physician assistant). Once you get a referral, make the call! You’ll be one step closer to successfully managing your diabetes.
If you don’t know of a diabetes education program, use our locator tool to find an accredited DSMES program near you.
Meeting with a
diabetes care and education specialist is a great first step, but
effective diabetes education is a process and takes time. It’s important to
attend all your DSMES appointments. If you need to miss an appointment, be sure
to reschedule.
Remember to discuss what you’ve learned with the medical
provider who referred you to the diabetes care and education specialist. As you
update them, they may be able to contribute helpful ideas. Managing diabetes is
a team effort.

Key Times for DSMES
Anytime is a good time to book an appointment with a diabetes care and education specialist (DCES), but there are a few times in your life when seeing one is extra important:
● When you’re diagnosed with diabetes
● At least once a year or when you’re struggling to meet your care goals
● When new complicating factors arise, such as changes in physical and emotional health or basic survival needs
● During significant life transitions and access to care
7 Key Areas
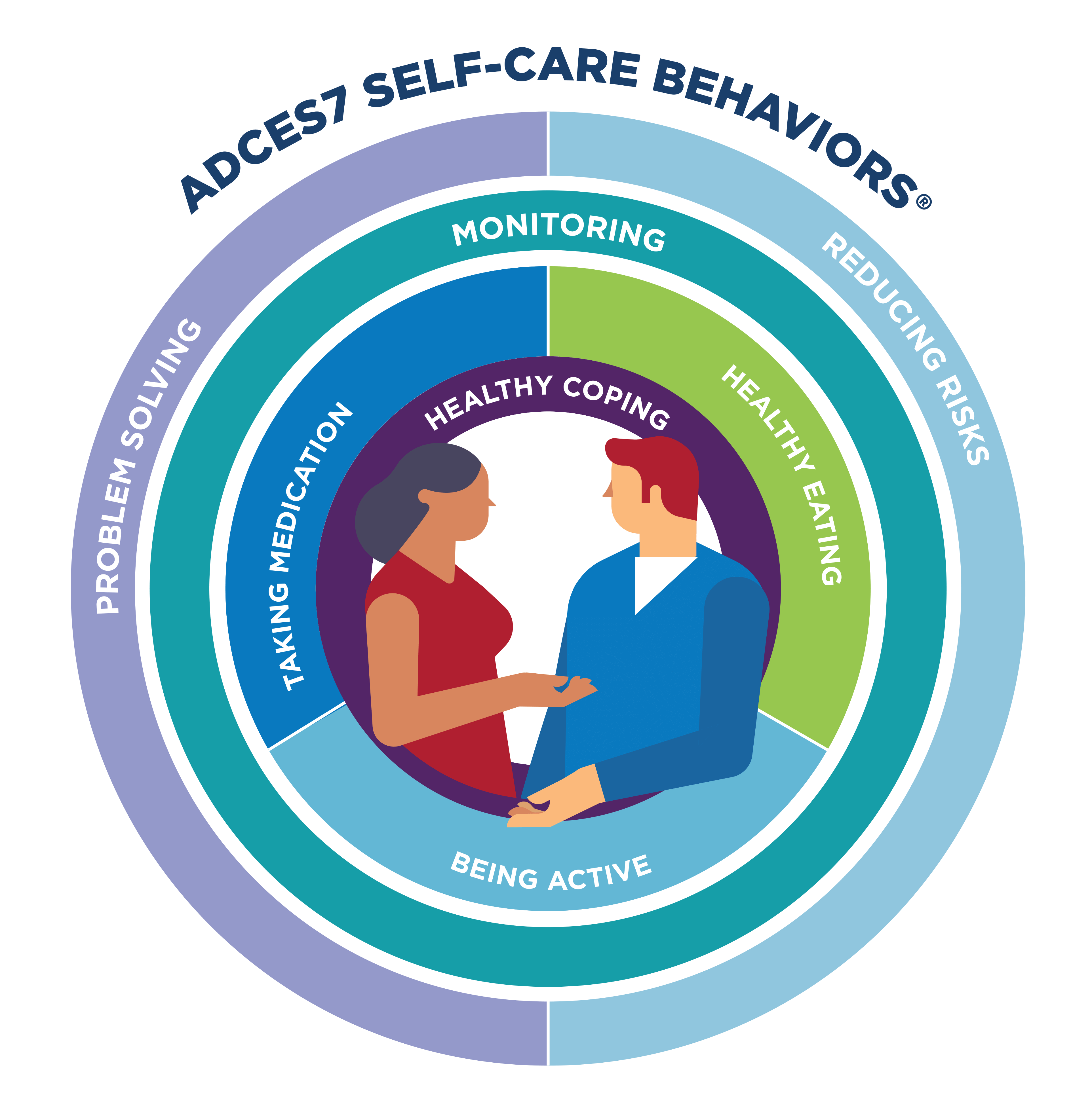
ADCES7 Self-Care Behaviors
Diabetes care and education specialists focus on seven self-care behaviors, known as the ADCES7 Self-Care Behaviors®, that are essential for improved health and greater quality of life; for example, eating healthy, taking medication and more.


